US DRUG CZAR EXPLAINS CAUSES AND RSDT TOOL TO PREVENT TEEN DRUG USE AND OVERDOSE DEATH INTERVIEW WITH U.S. DRUG CZAR JOHN WALTERS
Introduction: In response to recent news of a huge increase in drug overdose deaths and arrests for drug trafficking among Fairfax County youths, Fox News TV5 reporter Sherri Ly interviewed U.S. Drug Czar John Walters for his expert views on the cause and potential cure for these horrific family tragedies. Following is a transcript of that half-hour interview with minor editing for clarity and emphasis added. The full original interview is available through the 11/26/08 Fox5 News broadcast video available at link:
WALTERS: Well, as this case shows, while we’ve had overall drug use go down, we still have too many young people losing their lives to drugs, either through overdoses, or addiction getting their lives off track. So there’s a danger. We’ve made progress, and we have tools in place that can help us make more progress, but we have to use them.
Q 1: You meet with some of these parents whose children have overdosed. What do they tell you, and what do you tell them?
WALTERS: It’s the hardest part of my job; meeting with parents who’ve lost a child. Obviously they would give anything to go back, and have a chance to pull that child back from the dangerous path they were on. There are no words that can ease their grief. That’s something you just pray that God can give them comfort. But the most striking thing they say to me though is they want other parents to know, to act. And I think this is a common thing that these terrible lessons should teach us.
Many times, unfortunately, parents see signs: a change in friends, sometimes they find drugs; sometimes they see their child must be intoxicated in some way or the other. Because it’s so frightening, because sometimes they’re ashamed – they hope it’s a phase, they hope it goes away – they try to take some half measures. Sometimes they confront their child, and their child tells them – as believably as they ever can – that it’s the first time. I think what we need help with is to tell people; one, it’s never the first time. The probability is low that parents would actually recognize these signs – even when it gets visible enough to them – because children that get involved in drugs do everything they can to hide it. It’s never the first time. It’s never the second time. Parents need to act, and they need to act quickly. And the sorrow of these grieving parents is, if anything, most frequently focused on telling other parents, “Don’t wait: do anything to get your child back from the drugs.”
Secondly, I think it’s important to remember that one of the forces that are at play here is that it’s their friends. It’s not some dark, off-putting stranger – it’s boyfriends, girlfriends. I think that was probably a factor in this case. And it’s also the power and addictive properties of the drug. So your love is now being tested, and the things you’ve given your child to live by are being pulled away from them on the basis of young love and some of the most addictive substances on earth. That’s why you have to act more strongly. You can’t count on the old forces to bring them back to safety and health.
Q 2: When we talk about heroin – which is what we saw in this Fairfax County drug ring, alleged drug ring – what are the risks, as far as heroin’s concerned? I understand it can be more lethal, because a lot of people don’t know what they’re dealing with?
WALTERS: Well it’s also more lethal because one, the drug obviously can produce cardiac and respiratory arrest. It’s a toxic substance that is very dangerous. It’s also the case that narcotics, like heroin – even painkillers like OxyContin, hydrocodone, which have also been a problem – are something that the human body gets used to. So what you can frequently get on the street is a purity that is really blended for people who are addicted and have been long time addicted. So a person who is a new user or a naïve user can more easily be overdosed, because the quantities are made for people whose bodies have adjusted to higher purities, and are seeking that effect that only the higher purity will give them in this circumstance. So it’s particularly dangerous for new users. But we also have to remember, it almost never starts with heroin. Heroin is the culmination here. I think some of the – and I’ve only seen press stories on this — some of these young people may have gotten involved as early as middle school.
We have tools so that we don’t have to lose another young woman like this– or young men. We now have the ability to use Random Student Drug Testing (RSDT) because the Supreme Court has, in the last five years, made a decision that says it can’t be used to punish. It’s used confidentially with parents. We have thousands of schools now doing it since the president announced the federal government’s willingness to fund these programs in 2004. And many schools are doing it on their own. Random testing can do for our children what it’s done in the military, what it’s done in the transportation safety industry– significantly reduce drug use.
First, it is a powerful reason not to start. “I get tested, I don’t have to start.” We have to remember, it’s for prevention and not a “gotcha!” But it’s a powerful reason for kids to say, even when a boyfriend or girlfriend says come and do this with me, “I can’t do it, I get tested. I still like you, I still want to be your friend; I still want you to like me, but I just can’t do this,” which is very, very powerful and important. And second, if drug use is detected the child can be referred to treatment if needed.
Q 3: Is the peer pressure just that much that without having an excuse, that kids are using drugs and getting hooked?
WALTERS: Well one of the other unpleasant parts of my job is I visit a lot of young people in treatment; teenagers, sometimes as young as 14, 15, but also 16, 17, 18. It is not uncommon for me to hear from them, “I came from a good family. My parents and my school made clear what the dangers were of drugs. I was stupid. I was with my boyfriend (or girlfriend) and somebody said hey, let’s go do this. And I started, and before I knew it, I was more susceptible.”
We have to also understand the science, which has told us that adolescents continue to have brain development up through age 20-25. And their brains are more susceptible to changes that we can now image from these drugs. So it’s not like they’re mini-adults. They’re not mini-adults. They’re the particularly fragile and susceptible age group, because they don’t have either the experience or the mental development of adults. That’s why they get into trouble, that’s why it happens so fast to them, that’s why it’s so hard for them to see the ramifications.
So what does RSDT do? It finds kids early– if prevention fails. And it allows us to intervene, and it doesn’t make the parent alone in the process. Sometimes parents don’t confront kids because kids blackmail them and say “I’m going to do it anyway, I’m going to run away from home.” The testing brings the community together and says we’re not going to lose another child. We’re going to do the testing in high school – if necessary, in middle school. We’re going to wrap our community arms around that family, and get those children help. We’re going to keep them in school, not wait for them to drop out. And we’re certainly not going to allow this to progress until they die.
Q 4: And in a sense, if you catch somebody early, since you’re saying the way teenagers seem to get into drug use is a friend introduces it to a friend, and then next thing you know, you have a whole circle of friends doing it. Are you essentially drying that up at the beginning, before it gets out of hand?
WALTERS: That is the very critical point. It’s not only helping every child that gets tested be safer, it means that the number of young people in the peer group, in the school, in the community that can transfer this dangerous behavior to their friends shrinks. This is communicated like a disease, except it’s not a germ or a bacillus. It’s one child who’s doing this giving it behaviorally to their friends, and using their friendship as the poison carrier here. It’s like they’re the apple and the poison is inside the apple. And they trade on their friendship to get them to use. They trade on the fact that people want acceptance, especially at the age of adolescence. So what you do is you break that down, and you make those relationships less prone to have the poison of drugs or even underage drinking linked to them. And of course we also lose a lot of kids because of impaired driving.
Q 5: And how does the drug testing program work, then, in schools– the schools that do have it. Is it completely confidential? Are you going to call the police the minute you find a student who’s tested positive for heroin or marijuana or any other illicit drug?
WALTERS: That’s what is great about having a Supreme Court decision. It is settled – random testing programs cannot be used to punish, to call law enforcement; they have to be confidential. So we have a uniform law across the land. And what the schools that are doing RSDT are seeing is that it’s an enormous benefit to schools for a relatively small cost. Depending on where you are in the country, the screening test is $10-40. It’s less than what you’re going to pay for music downloads in one month for most teenage kids in most parents’ lives. And it protects them from some of the worst things that can happen to them during adolescence. Not only dying behind the wheel, but overdose death and addiction.
Schools that have done RSDT have faced some controversy; so you have to sit down and talk to people; parents, the media, young people. You have to engage the community resources. You’re going to find some kids and families that do have treatment needs. But with RSDT you bring the needed treatment to the kids.
I tell, a lot of times, community leaders – mayors and superintendents, school board members – that if you want to send less kids into the criminal justice system and the juvenile justice system, drug test — whether you’re in a suburban area or in an urban area.
What does the testing do? It takes away what we know is an accelerant to self-destructive behavior: crime, fighting in school, bringing a weapon, joining a gang. We have all kinds of irrefutable evidence now – multiple studies showing drugs and drinking at a young age accelerate those things, make them worse, make them more violent, as well as increasing their risks of overdose deaths and driving under the influence. So drug testing makes all those things get better. And it’s a small investment to make everything else we do work better.
Again, drug testing is not a substitute for drug education or good parenting or paying attention to healthy options for your kid. It just makes all those things work better.
Q 6: And I know you’ve heard this argument before, but isn’t that big brother? Aren’t there parents out there who say to you, “I’m the parent: why are you going to test my child for drugs in school; that’s my job?”
WALTERS: I think that is the critical misunderstanding that we are slowly beginning to change by the science that tells us substance abuse is a disease. It’s a disease that gets started by using the drug, and then it becomes a thing that rewires our brain and makes us dependent. So instead of thinking of this as something that is a moral failing, we have to understand that this is a disease that we can use the kind of tools for public health – screening and interventions – to help reduce it.
Look, let me give you the counter example. It’s really not big brother. It’s more like tuberculosis. Schools in our area require children to be tested for tuberculosis before they come to school. Why do they do that? Because we know one, they will get sicker if they have tuberculosis and it’s not treated. And we can treat them, and we want to treat them. And two, they will spread that disease to other children because of the nature of the contact they will have with them and spreading the infectious agent. The same thing happens with substance abuse. Young people get sicker if they continue to use. And they spread this to their peers. They’re not secretive among their peers about it; they encourage them to use them with them. Again, it’s not spread by a bacillus, but it’s spread by behavior.
If we take seriously the fact that this is a disease and stop thinking of it as something big brother does because it’s a moral decision that somebody else is making, we can save more lives. And I think the science is slowly telling us that we need to be able to treat this in our families, for adults and young people. We have public health tools that we’ve used for other diseases that are very powerful here, like screening – and that’s really what the random testing is. We’re trying to get more screening in the health care system. So when you get a check up, when you bring your child to a pediatrician, we screen for substance abuse and underage drinking. Because we know we can treat this, and we know that we can make the whole problem smaller when we do.
Q 7: You have said there were about 4,000 schools across the country now that are doing this random drug testing. What can we see in the numbers since the Supreme Court ruling in 2002, as far as drug use in those schools, and drug use in the general population?
WALTERS: Well, what a number of those schools have had is of course a look at the harm from student drug and alcohol use. Some of them have put screening into place, random testing, because they’ve had a terrible accident; an overdose death; death behind the wheel. What’s great is when school districts do this, or individual schools do this, without having to have a tragedy that triggers it. But if you have a tragedy, I like to tell people, you don’t have to have another one. The horrible thing about a tragic event is that most people realize those are not the only kids that are at risk.
There are more kids at risk, obviously, in our communities in the Washington, DC area where this young woman died. We know there’s obviously more children who are at risk of using in middle school and high school. The fact is those children don’t have to die. We cannot bring this young lady back. Everybody knows that. But we can make sure others don’t follow her. And the way we can do that is to find, through screening, who’s really using. And then let’s get them to stop – let’s work with their families, and let’s make sure we don’t start another generation of death. So what you see in these areas is an opportunity to really change the dynamic for the better.
Q 8: Now, although nationally drug use among our youth is going down – what does it say to you – when I look at the numbers specific to Virginia, the most recent that I could find tells me that 3% of 12th graders, over their lifetime, have used a drug like heroin? What does it say to you? To me, that sounds like a lot.
WALTERS: Yeah, and it’s absolutely true. I think the problem here is that when you tell people we are taking efforts that are making progress nationwide, they jump to the conclusion that that means that we don’t have a problem anymore. We need to continue to make this disease smaller. It afflicts our young people. It obviously also afflicts adults, but this is a problem that starts during adolescence — and pre-adolescence in some cases — in the United States. We can make this smaller. We not only have the tools of better prevention but also better awareness and more recognition of addiction as a disease. We need to make that still broader. We need to use random testing. If we want to continue to make this smaller, and make it smaller in a permanent way, random testing is the most powerful tool we can use in schools.
We want screening in the health care system. We have more of that going on through both insurance company reimbursement and public reimbursement through Medicare and Medicaid for those who come into the public pay system. That needs to grow. It needs to grow into Virginia, it’s already being looked at in DC; it needs to grow into Maryland and the other states that don’t have it. We are pushing that, and it’s relatively new, but it’s consistent with what we’re seeing – the science and the power of screening across the board.
We need to continue to look at this problem in terms of also continuing to push on supply. We’re working to reduce the poisons coming into our communities, which is not the opposite of demand; that we have to choose one or the other. They work together. Keeping kids away from drugs and keeping drugs away from kids work together. And where we see that working more effectively, we’ll save more lives. So again, we’ve seen that a balanced approached works, real efforts work, but we need to follow through. And the fact that you still have too many kids at risk is an urgent need. Today, you have kids that could be, again, victims that you have to unfortunately tell about on tonight’s news, that we can save. It’s not a matter we don’t know how to do this. It’s a matter of we need to take what we know and make it reality as rapidly as possible.
Q 9: Where are these drugs coming from? Where’s the heroin that these kids allegedly got coming from?
WALTERS: We do testing about the drugs to figure out sources for drugs like heroin. Principally, the heroin in the United States today has come from two sources. Less of it’s coming out of Colombia. Colombia used to be a source of supply on the East Coast, but the Colombian government, as a part of our engagement with them on drugs, has radically reduced the cultivation of poppy and the output of heroin. There still is some, but it’s dramatically down from what it was even about five years ago. Most of the rest of the heroin in the United States comes from Mexico. And the Mexican government, of course, is engaged in a historic effort to attack the cartels. You see this in the violence the cartels have had as a reaction. So we have promising signs. There are dangerous and difficult tasks ahead, but we can follow through on that as well.
Most of the heroin in the world comes from Afghanistan; 90% of it. And we are working there, of course, as a part of our effort against the Taliban and the forces of terror and Al Qaeda, to shrink that. The good news is that last year we had a 20% decline in cultivation and a 30% decline in output there. Most of that does not come here, fortunately. But it has been funding the terrorists. It’s been drained out of most of the north and the east of the country. It’s focused on the area where we have the greatest violence today, in the southwest. We’re working now – you see Secretary Gates talking to the NATO allies about bringing the counter-insurgency effort together with the counter-narcotics effort to attack both of these cancers in Afghanistan. We have a chance to change heroin availability in the world in a durable way by being successful in Afghanistan. We’ve started that path in a positive way. Again, it’s a matter of following through as rapidly as possible.
Q 10: Greg Lannes, the father of the girl in Fairfax County who died, told me that one of his main efforts, as you imagined, was to let people know that those drugs, they’re coming from where it is produced, outside our country; that they’re getting all the way down to the street level and into our neighborhoods– something that people don’t realize. So when you hear that they busted a ring of essentially teenagers who have been dealing, using and buying heroin, what does that say to you as the man in charge of combating drugs in our country?
WALTERS: Well again, we have tools that can make this smaller. But we have to use those tools. And we have multiple participants here. Yes we need to educate. And we need to make sure that parents know they need to talk to their children, even when their children look healthy and have come from a great home. Drugs – we’ve learned, I think, over the last 25 years or more, drugs affect everybody; rich or poor, middle class, lower class or upper class. Every family’s been touched by this, in my experience, by alcohol or drugs. They know that reality– we don’t need to teach them that.
What we need to teach them is the tools that we have that they can help accelerate use of. Again, I think – there is no question in my mind that had this young woman been in a school, middle school or high school that had random testing – since that’s where this apparently started, based on the information I’ve seen in the press – she would not be dead today. So again, we can’t go back and bring her to life. But we can put into place the kind of screening that makes the good will and obvious love that she got from her parents, the obvious good intentions that I can’t help but believe were a part of what happened in the school, the opportunities that the community has to have a lot of resources that she didn’t get when she needed them. And now she’s dead. Again, we can stop this: we just have to make sure we implement that knowledge in the reality of more of our kids as fast as possible.
Q 11: Should anyone be surprised by this case? And that such a hardcore drug like heroin is being used by young people?
WALTERS: We should never stop being surprised when a young person dies. They shouldn’t die. They shouldn’t die at that young age, and we should always demand of ourselves, even while we know that’s sometimes going to happen today, that every death is a death too many. I think that it is very important not to say we’re going to accept a certain level. Never accept this. Never! That’s my attitude, and I know that’s the president’s attitude as well here. Never accept that heroin’s going to get into the lives of our teenagers. Never accept that our children are going to be able to use and not be protected. It’s our job to protect them. They have a role, also, obviously in helping to protect themselves. But we need to give them the tools that will help protect them.
When I talk to children and young adults in high school or college, they know what’s going on among their peers. And in some ways, when you get them alone and they feel they can talk candidly, they tell us they don’t understand why we, as adults who say this is serious, don’t act. They know that we see children who are intoxicated; they know that we must see signs of this, because as kid’s lives get more out of control, they show signs of it. They want to know why we don’t act.
We can use the tools of screening, and we can use the occasion of a horrible event like this to bring the community together and say it’s time for us to use the shock and the sorrow for something positive in the future. I haven’t met a parent of a child who’s been lost who doesn’t say I just want to use this now for something positive. And that’s understandable, and I think we ought to honor that wish.
Q 12: Well, I guess I’m not asking should we accept that this is in our schools, but is it naïve for people not to understand or realize that these hardcore drugs are in our schools, and in our communities, and in our neighborhoods.
WALTERS: Yeah. Where it is naïve, I think, is to not recognize the extent and access that young people have to drugs and alcohol. I think we sometimes think that because they come from a home where this isn’t a part of their lives now, that it’s not ever going to be part of their lives. Look, your viewers should go on the computer. Type marijuana into the Google search engine and see how many sites encourage them to use marijuana, how to get marijuana, how to grow marijuana, the great fun of marijuana. Go on YouTube and type in marijuana, and see how many videos come up using marijuana, joking around about marijuana. And then when you start showing one, of course the system is designed to show you similar things. Type in heroin. See what kind of sites come up, and see what kind of videos come up on these sites. Young people spend more time on these sites than they do, frequently, watching television. Remember, there is somebody telling your children things about drugs. And if it’s not you, the chances are they’re telling them things that are false and dangerous. So there is a kind of naiveté about what the young peoples’ world, as it presents itself to them, tells them about these substances. It minimizes the danger, it suggests that it’s something that you can do to be more independent, not be a kid anymore.
We, from my generation — because I’m a baby boomer — unfortunately have had an association of growing up in America with the rebellion that’s been associated with drug use. That’s been very dangerous, and we’ve lost a lot of lives. We have to remember that it’s alive and well, and has become part of the technological sources of information that young people have. I also see young people in treatment centers who got in a chat room and somebody offered them drugs or offered them to come and buy them alcohol and flattered them, and got them involved in incredibly self-destructive behavior. The computer brings every predator and every dangerous influence into your own child’s home – into their bedroom in some cases, if that’s where that computer exists. You wouldn’t let your kids go out and play in the park with drug dealers. If you have a computer and it’s not supervised, those drug dealers are in that computer. Remember that. And they’re only a couple of keystrokes away from your child.
Q 13: And you talk about the YouTube and the computers and all those things. What about just the overall societal image? Because we have this whole image with heroin, of heroin chic. How much does that contribute to the drug use, and how difficult does it make your job, when a drug is being made out to be cool in society by famous people?
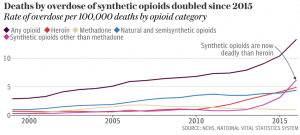
WALTERS: There are still some elements of that. It was more prominent a number of years ago. I would say you see less of that now glamorized in the entertainment industry, or among people who are celebrities in and out of entertainment. You see more cases of real harm. But it’s still out there. The one place that I think is replacing that, just to get people ahead of the game here, is prescription pharmaceuticals. Those have been marketed to kids on the internet as a safe high. They falsely suggest that you can overcome the danger of an overdose because you can predict precisely the dosage of OxyContin, hydrocodone, Vicodin. And there are sites that suggest what combination of drugs to use. We’ve seen prescription drug use as the one counter example of a category of drug use going up among teens. We’re trying to work on that as well, but that’s something that’s in your own home, because many people get these substances for legitimate medical care. Young people are going to the medicine cabinet of family or friends, taking a few pills out and using those. And those are as powerful as heroin, they’re synthetic opioids, and they have been a source of overdose deaths.
So let’s not forget – while this Fairfax example reminds us of the issues of heroin chic and of the heroin that’s in our communities, the new large problem today is a similar dangerous substance in pill form in our own medicine cabinets. Barrier to access is zero. They don’t have to find a drug dealer; they just go find the medicine cabinet. They don’t have to pay a dime for it because they just take it and they share that with their friends. We need to remember, that’s another dimension here. Keep these substances out of reach – under our control when we have them in our home. Throw them away when we’re done with them. Make sure we talk to kids about pills. Because people, again, are telling them that’s the place to go to avoid overdose death, is to take a pill.
Q 14: When you see a lot of these celebrities checking in and out of rehab, does it sort of glamorize it for kids? And teach them hey, you can use, you can check into rehab, you can come back, you can – you know. Is there a mixed message there?
WALTERS: There is. Some young people interpret it the way you describe; of it’s something you do and you can get away with it by going into rehab. We do a lot of research on young people’s attitudes for purposes of helping shape prevention programs in the media, as well as in schools and for parents. We do a lot with providing material to parents. I would say that compared to where we’ve been in the last 15 or 20 years, there’s less glamorization today.
I think we should also remember the positive, because we reinforce that. A lot of young people – obviously not all or we wouldn’t have this death – believe that taking drugs makes you a loser. They’ve seen that a lot of those celebrities are showing their careers going down the toilet because they can’t get away from the pills and the drugs and the alcohol. And I think they see that even among some of their peers. That’s a good thing. We should reinforce that as parents: teaching our kids that drug and alcohol use may be falsely presented to you as something you do that would make you popular, make you seem like you should have more status in society generally. But actually, look at a lot of these people; they’ve had enormous opportunities, enormous gifts, and they can’t stop themselves from throwing them away. And they may not stop themselves from throwing away their lives.
I think you could use these events as a teachable moment. It can go two ways. Help your child understand what the truth is here. And I tell young people – and I think parents have to start this more directly – this is the way this is going to come to you: Somebody you really, really want to like you; somebody you really, really like; someone you may even love — or think you love — they’re going to say come and do this with me. If you can’t find any other reason to not do this with them, say, “Before we do this, let’s go to a treatment center. Let’s go talk to people who stood where we stood and said it’s not going to happen to me.” If everybody, when they got the chance to start, thought of an addict or somebody who was dead, they wouldn’t start. The fact is that does not enter their mind.
Many people in treatment centers understand that part of the task of recovery is helping other people avoid this. So they’re willing to talk about it. In fact, that’s part of their path of staying clean and sober, which not many kids are going to be able to do on their own. But it makes them think that what presents itself as something overwhelmingly attractive has behind it a horrible dimension, for their friends as well as for themselves. And more and more, I think kids understand this.
We can use the science of this as a disease, and the experience of many families. Remember, uncle Joe didn’t used to be like this. Especially Thanksgiving, when we have families getting together and all of a sudden mom’s going to get loaded and become ugly in the corner. We also have to remember we have an obligation to reach out to those people, and to get them help. We can treat them. Nobody gets sober, in my experience, by themselves. They have to take responsibility. But you have to overcome the pushback, and addiction and alcoholism have, as a part of the disease, denial. When you tell somebody they have a problem, they get angry with you. They don’t say hey thanks, I want your help. They don’t hit bottom and become nice. That’s a myth. They need to be grabbed and encouraged and pushed. Almost everybody in treatment is coerced – by a family member, by an employer, sometimes by the criminal justice system.
So remember that, when you find your child using and they want to lie to you up down and sideways saying, “It’s the first time I’ve ever done it.” No, no, no, no, no, that’s the drugs talking. That shows you, if anything, you have a bigger problem than you realized and you need to reach out, get some professional help. But don’t wait!
Source: National Institute of Citizen Anti-drug Policy (NICAP)
DeForest Rathbone, Chairman, Great Falls, Virginia, 703-759-2215, DZR@prodigy.net